The Health Budget and Neoliberal Ideology
09/05/2013
In the past two years the UPA government, with considerable fanfare, has attempted to project a view that it is serious about bringing about radical changes as regards access to health care.
A slew of measures have been announced, and considerable debate was generated in the past year regarding plans to put in place a system that would ensure Universal Health care. With a year (or less) to go until the next general elections, it is necessary to examine to what extent the government has redeemed its promise.
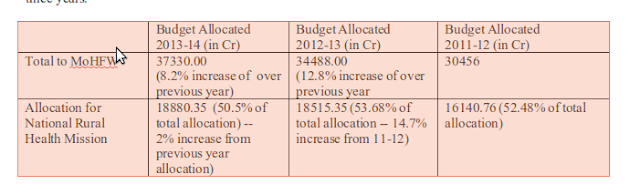
The most immediate indication of the government’s true intent is this year’s budget, and specifically the health budget. The Table below provides the overall figures for budgetary allocation on health in the past three years.
Significant decrease in allocation for the National Health Mission
Several important issues stand out if we look at the figures. First, there has been a mere 8.2% increase in total allocation. This increase must be seen in several contexts. It needs to be contrasted with the promise in the 12th Five Year Plan that allocation for health, would be increased by 300% over the allocation for the 11th Plan. In other words the 12th Plan projects an increase of around 60% every year, over the previous year’s allocation. The present increase, however, is barely enough to cover for inflation, meaning that there has been no actual increase proposed. In his budget speech the Finance Minister had announced that he is proposing a 22% increase. The discrepancy arises as he was referring to the revised estimates – which over the last few years have always been lower than the budget allocation in the case of social sector spending. So we can actually expect a much lower allocation than what is proposed in the current budget.
More intriguingly, if we adjust for inflation, the 2% increase for the National Rural Health Mission actually translates into a decrease in real allocation. This is so despite the announcement that the NRHM shall now include two new components – a flexi-pool for communicable disease control and for urban health (previously not covered by the NRHM, and hence leading to the proposal to rename the NRHM as the National Health Mission). It is an indication of the way the government of the day functions that it believes that it is perfectly rational to announce an expansion of a government programme, and at the same time actually propose a cut in the budget!
The story does not end here. There is no extra allocation for the ‘free medicines’ scheme that was announced a year and half back by no less a person than the Prime Minister of India. This announcement was received with enthusiasm both nationally and internationally, with even the World Health Organisation showcasing it as a model for other countries to follow. 18 months down the line it has remained just that, an announcement. Only a government that has now lost the need to even keep up pretences, can brazenly keep silent about a programme that its own ministers and officials have projected as an “achievement” of the UPA II Government. If the free medicines scheme was to be operationalised, the health ministry’s own estimates is that it would require an additional allocation of Rs.6,000 crores every year.
Consider another piece of doublespeak by the government. The UPA I government, in its common minimum programme in 2004, had said it would increase spending on health to 2-3% of GDP. The same was echoed by the 11th Five Year Plan document and again by the High Level Expert Group (HLEG) set up in 2011 by the government (see later). Yet the 12th Five Year Plan talks of increasing health expenditure to 1.87% of GDP (if realized would still keep India firmly among the bottom 5% of nations). So, after 9 years, after several rounds of reiteration, the 12th Plan actually recommends reducing our aspirations regarding public spending on health. It is of course another matter that health spending has remained stubbornly at around 1% of GDP and given the direction in the current budget, it is unlikely to change.
The mirage called Universal Health Care
This year’s health budget is, in fact, the tail end of a longer story. Two years back the government, accompanied by considerable publicity, had announced the setting up of a High Level Expert Group (HLEG), tasked to recommend ways in which the country could achieve Universal Health Care (UHC). UHC, by this time, had already become a buzzword in international circles. Proposed in a World Health Assembly resolution in 2005, UHC has now become the new jargon among health planners across the world. Unfortunately, UHC has come to mean different things for different people as there has never been any conceptual clarity regarding what UHC means, To some UHC was quickly converted to Universal Health Coverage (rather than care) and then further coverage was taken to mean coverage by a limited insurance based package, and not access to comprehensive health services. There was a very deep game that was played out, and there was a deliberate ploy to limit the discussion to the financing of UHC and not to how health care would actually be provided.
Unfortunately the HLEG report walked right into this trap. The report made several useful recommendations, including recommendations to abolish user fees; to move from selective health care to comprehensive health care; and to replace a system where only BPL was eligible for free care to where almost everyone was entitled to free care. But caught up, as it was, in the current jargon of UHC, the HLEG did not unambiguously recommend that universal care, to be accessible to all, must ultimately be provided by public health facilities. Instead the HLEG hedged its bets and left the door open for the possibility of private sector participation, in a systematic manner, in the entire schema of UHC. The report said: “State governments should consider experimenting with arrangements where the state and district purchase care from an integrated network of combined primary, secondary and tertiary care providers”. What is remarkable about this recommendation (para 3.1.10 of the HLEG report) is that there is a clear attempt to keep ambiguous the question as to who the ‘integrated network’ would actually represent.
Clearly, however, the Planning Commission did not see any ambiguity. It gleefully pounced on the paragraph, and it became the major part of the HLEG’s recommendations that the Planning Commission selectively quoted. The Planning Commission of India led by one of the foremost practitioners of neoliberal economics in India, understood the phrase ‘integrated network’ to mean a network that was run by a private entity! Thus the initial draft of the health chapter of the 12th Plan document went on to elaborate its grand plan of handing health care over to the corporate sector, very akin to the disastrous ‘managed care’ model in the United States.
Fortunately the Planning Commission’s wishes did not entirely fructify. Several organisations, including the Jan Swasthay Abhiyan, and even the government’s own Ministry of Health, objected to this formulation. Eventually the notion was watered down in the final 12th Plan document to a recommendation that pilot programmes on UHC would be run during the Plan period in some districts.
Attempt to delegitimise the Public Health system
Neoilibral economics is an aggressive ideology – it does not respect popular sentiment, nor does it back off in the face of adversity. Stymied temporarily in its attempt to hand over the health sector to managed care by corporations, it has struck back in the 2013-14 budget. The current budget is a shameless attempt to denude and disrupt the public heath system, and thereby delegitimise it further. The public system in India continues to be plagued by several problems. But it is important to understand that the foremost problem is that it is under financed and under-resourced. The modest increase in resource allocation to the NRHM had started making some inroads.
The public health system has continued to function in an adverse climate even after the launch of the NRHM. Since its launch, funds released have been only one third of the envisaged funds under the approved framework of the NRHM – about Rs.66,000 crore was released against Rs.175,000 crores envisaged. Funds released under 11th Plan are less than half of what was the original Plan outlay.
It is necessary to nail the lie that the public sector is inherently inefficient. Today, public health expenditure accounts for only 20% of total health expenditure and includes the services of only 20% of the country’s health workforce. Yet it provides for about 20% of all out-patient care (33% of all qualified out-patient care); 40% of all in-patient care, including about 60% of all hospital based critical pre-terminal care; and almost 100% of all preventive and promotive care. Inefficiencies as well as corruption do exist in the system. But these are not inherent faults of the system, they are introduced into the system by the same government that calls it inefficient. Evidence across the world shows that all the success stories in health care have their roots in public health systems – Cuba, Costa Rica, Sri Lanka, Thailand. In our own country the evidence states at us – states such as Kerala and Tamilnadu that have performed better have done so because they continued to invest in building public systems, often in spite of contrary signals from the central government.
The 2013-14 budget is a clear example of neoliberal political ideology striking back. It is an attempt to halt the little progress that the public health system has made in the past few years. The expectation is clear – with a deterioration of the already fragile public system, private players will find further opportunities to expand their activities. Who are these private players? No more do we see individual practitioners or even small nursing homes thriving. The new generation of private actors are networked chains of private hospital and their franchises, and insurance companies. They will be the ultimate gainers as long as ‘market fundamentals’ continue to determine if people will live or die.
